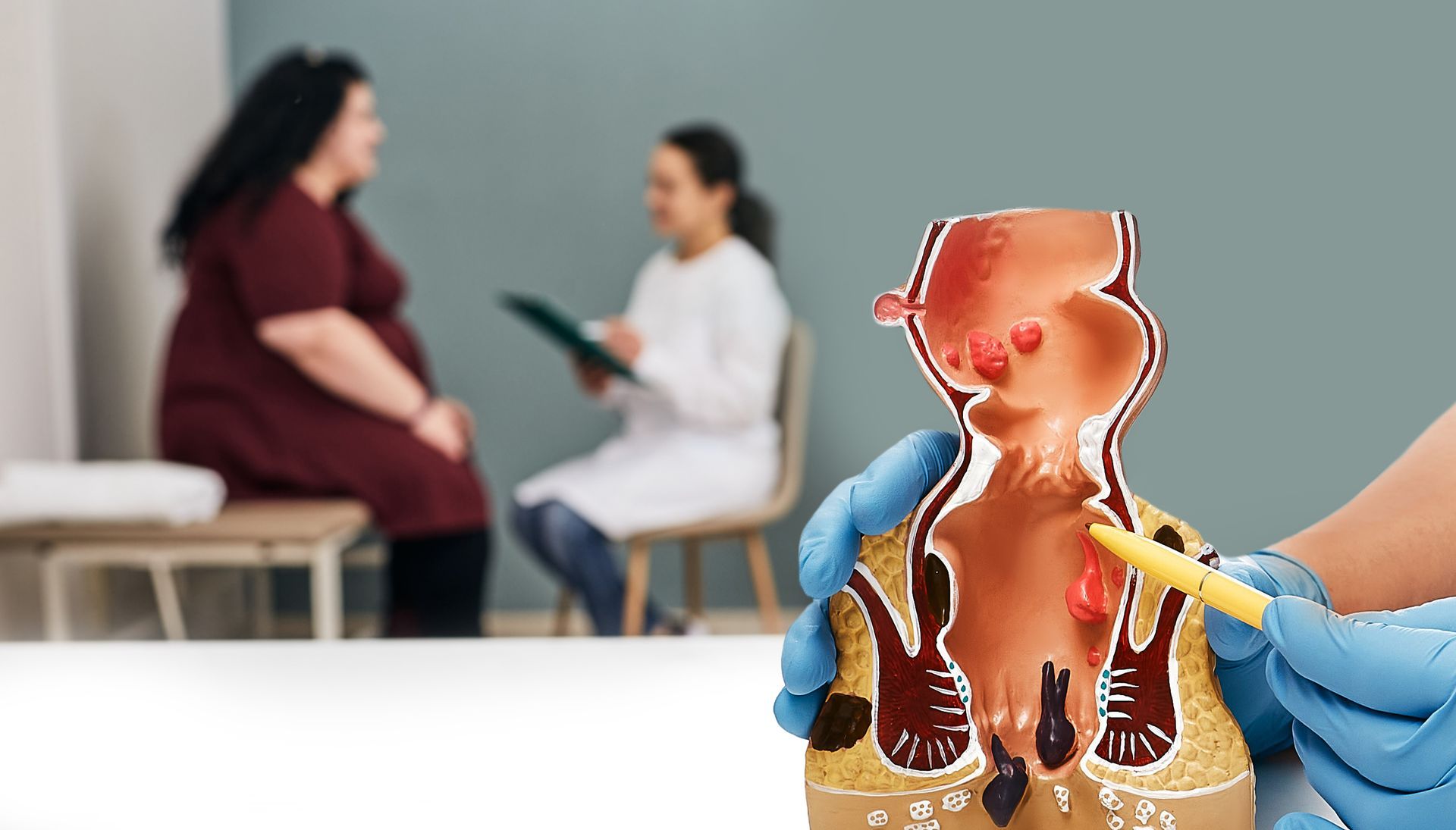
BARRETT'S ESOPHAGUS IN FLORIDA
With Barrett's esophagus, a type of tissue similar to that lining the intestines takes the place of the normal tissue lining the lower esophagus. Gastroesophageal reflux disease (GERD), a condition where stomach acid rushes back into the esophagus, is the main contributor to this alteration. This ongoing acid exposure has the potential to cause the esophagus to generate aberrant tissue over time.
HAVE QUESTIONS ABOUT BARRETT'S ESOPHAGUS?
-
What are the Signs and Symptoms of Barrett’s Esophagus?
Barrett's esophagus often has no symptoms at all. However, people may have heartburn, regurgitation, trouble swallowing, and a persistent cough, which are signs of chronic acid reflux. It is significant to remember that these symptoms might differ from person to person, and some people may not have any symptoms at all.
-
What are the Causes and Risk Factors for Barrett’s Esophagus?
GERD, which happens when the lower esophageal sphincter (LES) weakens or relaxes abnormally and permits stomach acid to flow backward into the esophagus, is the main contributor to Barrett's esophagus. The esophageal lining becomes inflamed and alterations in the cells occur as a result of the continual exposure to stomach acid.
The likelihood of having Barrett's esophagus may be impacted by a number of factors, including:
Long-term, severe GERD considerably increases the likelihood of developing chronic acid reflux. Middle-aged and older persons are also more likely to have Barrett's esophagus, and men are more likely to get it than women. Carrying around extra weight also increases strain on the abdomen, raising the risk of GERD.
Smoking inhibits the LES and hinders the esophagus' ability to recover. A condition known as a hiatal hernia can increase the risk of acid reflux by allowing the top portion of the stomach to protrude through the diaphragm. Family history is another factor that can increase the likelihood of developing this condition.
-
How do you Diagnosis and Treat Barrett’s Esophagus?
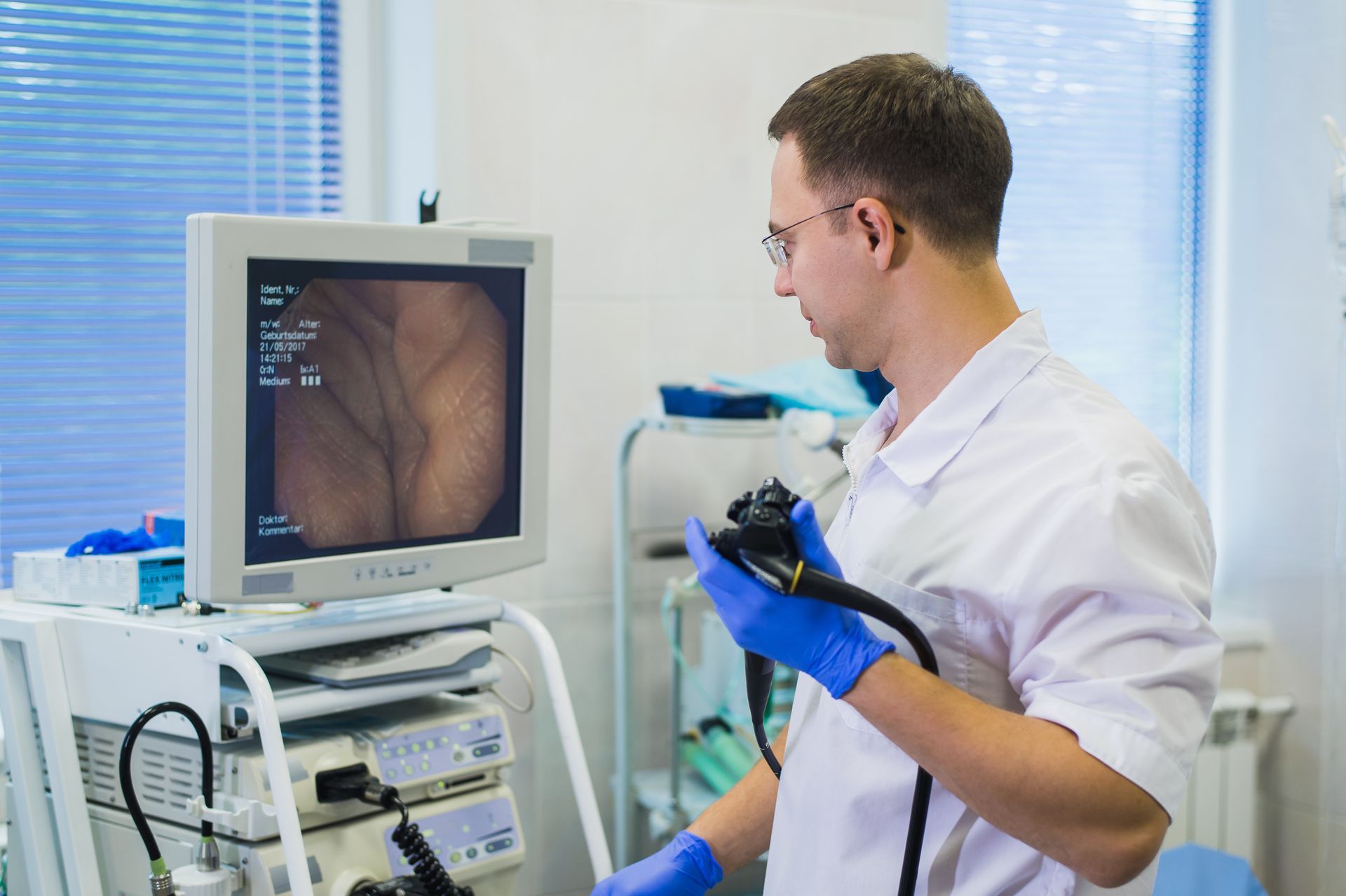
An upper endoscopy, which involves inserting a thin tube with a camera into the mouth and into the esophagus, is commonly used to diagnose Barrett's esophagus. A biopsy is performed during this process to evaluate the tissue and determine whether any aberrant cell alterations are present.
If Barrett's esophagus is identified, the type of treatment depends on how severe the problem is and whether dysplasia, a cell change that indicates cancer, is present. Options for treatment include:
Modifying one's lifestyle can help control symptoms and lessen acid reflux. Examples of such adjustments include giving up smoking, elevating the head of the bed, avoiding trigger foods, and maintaining a healthy weight.
Proton pump inhibitors (PPIs), H2 blockers, and over-the-counter antacids can all help symptoms and lessen acid production. Endoscopic surveillance can be used to track the development of Barrett's esophagus and look for any indications of dysplasia or early-stage cancer, routine endoscopic examinations may be advised.
Endoscopic therapies use cutting-edge endoscopic methods like radiofrequency ablation (RFA) or cryotherapy, aberrant tissue in the body can be removed or destroyed. Surgical intervention may be appropriate in severe cases or when dysplasia progresses to cancer, surgical options such as esophagectomy (removal of the esophagus) may be considered.
Barrett's esophagus is a condition that requires attention and appropriate management due to its potential progression to esophageal cancer. Recognizing the signs and symptoms, understanding the underlying causes and risk factors, and seeking early diagnosis are crucial steps in the effective treatment of this condition. By adopting lifestyle modifications, taking prescribed medications, and undergoing regular surveillance, individuals with Barrett's esophagus can mitigate the risks and ensure optimal long-term health. If you experience persistent acid reflux or related symptoms the expert staff of gastroenterologists at Digestive Diseases Center are here to help.
READY TO SCHEDULE AN APPOINTMENT?
RECENT POSTS
CONTACT
850-763-5409
ADDRESSES
4 LOCATIONS
204 E 19th Street, B, Panama City
12216 Panama City Beach Pkwy, D, Panama City Beach
4295 3rd Ave, Marianna
101 Good Morning St., 109B, Port St. Joe
Subscribe to our newsletter:
subscribe to our newsletter
We will get back to you as soon as possible.
Please try again later.